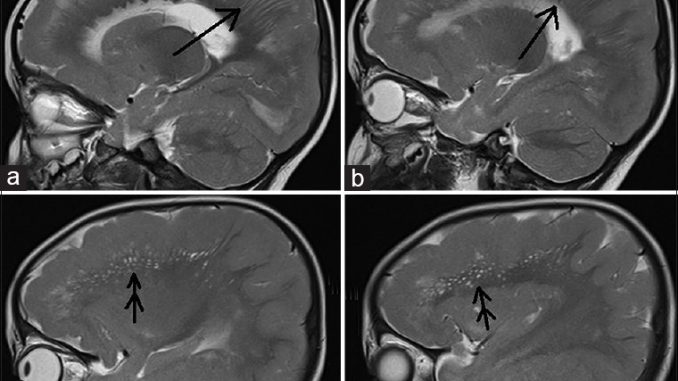
We report on 2 families with diffuse pachygyria and cerebellar hypoplasia, who presented hypotonia, ataxia, seizures, and developmental delay since infancy.
Computed tomography (CT) and magnetic resonance imaging (MRI) revealed decreased gyral formation in the cerebral cortex and marked hypoplasia in the cerebellum. Cerebellar hypoplasia is often associated with type 2 lissencephaly; however, our cases showed no polymicrogyria, and their clinical findings were quite mild compared with those of microlissencephaly. Their characteristic phenotype suggested a new genetic syndrome, which was possibly inherited as an autosomal recessive trait.
Kato, Mitsuhiro; Takizawa, Noboru; Yamada, Sirou; Ito, Aiko; Honma, Tomomi; Hashimoto, Motoya; Saito, Emi; Ohta, Tomoko; Chikaoka, Hideo; Hayasaka, Kiyoshi, 1999: Diffuse pachygyria with cerebellar hypoplasia A milder form of microlissencephaly or a new genetic syndrome?. Annals Of Neurology. 46(4): 660-663,.


